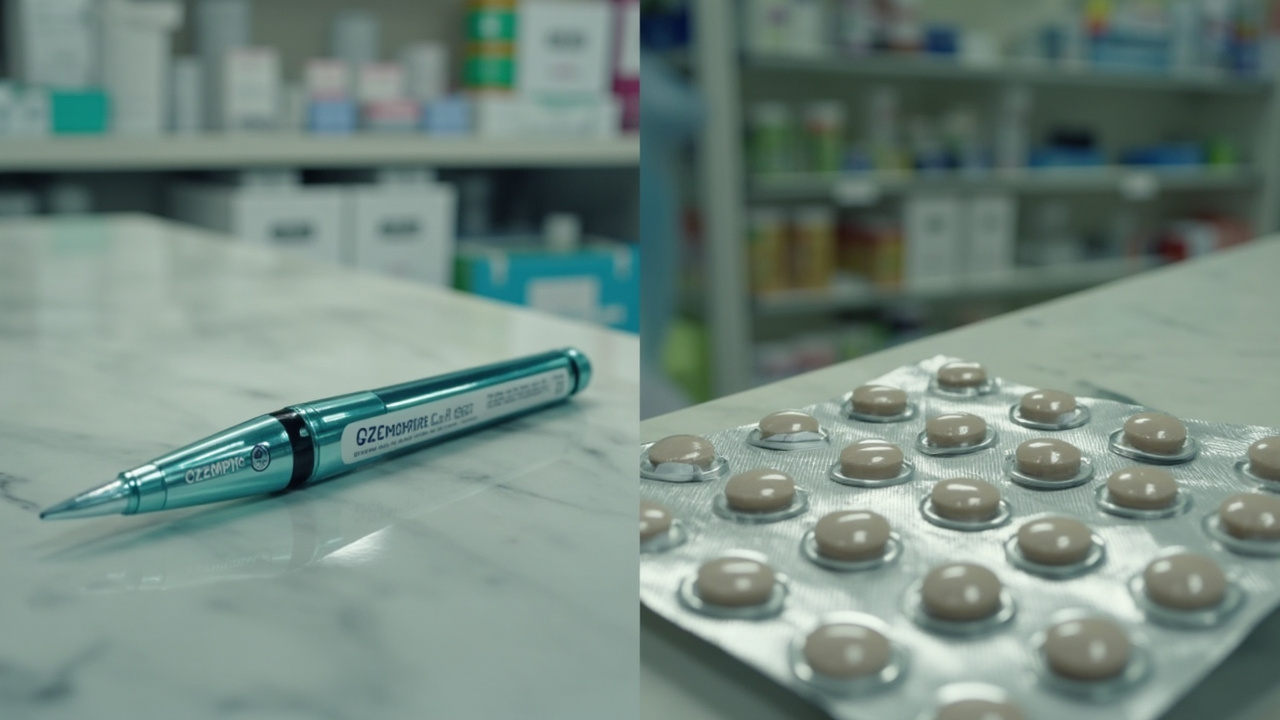
India's semaglutide patent expired March 20, and more than 50 generic drugmakers are launching versions at $14-40 a month — against America's $936 price tag.
Bloomberg leads with Natco's $14 generic launch; Reuters frames the expiry as a trigger for a wave of cheaper GLP-1 drugs across India and beyond.
X is framing the patent expiry as a moral indictment of US drug pricing, with posts contrasting $936 American Ozempic against $14 Indian generics going viral across continents.
Novo Nordisk's Indian patent on semaglutide — the molecule behind Ozempic and Wegovy — expired on March 20. Within hours, at least five Indian pharmaceutical companies began shipping generic versions at prices ranging from $14 to $40 a month. [1] In the United States, a month's supply of branded Ozempic costs $936. [2] The math is not complicated. The implications are.
India is the world's largest supplier of generic medicines, providing roughly 20 percent of global supply. [3] Companies including Natco Pharma, Eris Lifesciences, Sun Pharma, and Dr. Reddy's Laboratories have regulatory approval from India's drug controller and were waiting for the patent clock to run out. [4] More than 50 branded generic versions are expected to reach the Indian market in the coming weeks, according to NDTV, creating what India Today called a "launch storm." [5] Natco's injectable version will sell for approximately 1,200 rupees — about $14 — for the lowest monthly dose. [6]
The price gap between the American branded product and its Indian generic equivalent is not a rounding error. It is a 67-to-1 ratio. A JAMA-published study from March found that injectable semaglutide could be manufactured for as little as $3 per month — roughly $28 to $140 per year — if produced at scale. [7] The Guardian reported on the study's conclusion: the drug that reshaped American beauty standards and generated $18 billion in annual revenue for Novo Nordisk could, in theory, be made available to diabetics and obesity patients across 160 countries at a fraction of what wealthy nations currently pay. [8]
This is where the pharma story becomes a body politics story. Semaglutide did not stay in endocrinology clinics. It migrated to Hollywood, to Instagram, to dinner party conversations about who looks different and why. The drug became shorthand for a new era of chemical weight management — controversial among eating disorder specialists, celebrated among patients with Type 2 diabetes, and aspirational for millions who could not afford it. That last group just got considerably larger.
The Indian generics will not be available in the United States, where Novo Nordisk's patent protections extend years longer. But the existence of a $14 version of a $936 drug applies a specific kind of pressure. Compounding pharmacies in the US were already producing semaglutide copies under FDA enforcement discretion during the drug shortage; the FDA's decision on whether to continue allowing compounding now carries the additional weight of a global market where the identical molecule costs less than a large pizza. [9]
On X, the reaction has been less about pharmaceutical regulation than about national humiliation. Posts comparing the two price points have gone viral across India, the US, and Europe, with users treating the gap as a referendum on American healthcare. [10] The framing is simple and effective: India, a country with a per capita GDP of $2,500, will sell you the same drug that costs an American with insurance a $25 copay and an American without insurance a second mortgage.
For Novo Nordisk, the Indian market was never the revenue center — the US and Europe are. But generics have a way of crossing borders, through medical tourism, online pharmacies, and the slow diplomacy of price benchmarking. The $936 price was always a fact of patent law, not production cost. Now the patent has expired somewhere, and the production cost is public knowledge. The question is how long the distance between $3 and $936 remains politically sustainable.